
The mean sac diameter of the gestational sac is 10.6 mm. Am J Obstet Gynecol 161:747, 1989)įig 1A A very early, 3-mm mean diameter intrauterine gestational sac at 5 weeks postmenstruationįig 1B A typical yolk sac. (Warren WB, Timor-Trisch I, Peisner DB et al: Dating the early pregnancy by sequential appearance of embryonic structures. LMP, last menstrual period +FHTs, positive fetal heart tones Table 1 The appearance of early gestational structures The practitioner must understand that these β-hCG levels are guidelines for the appearance of these structures and are not 100% reliable or accurate. Suffice it to say that the presently used Third International Standard and Fourth International Standard, used by most companies marketing β-hCG kits, corresponds roughly to the First International Reference Preparation. 2 The literature regarding the correlation between quantitative β-hCG titers and early intrauterine gestational sacs and embryonic structures has been made somewhat confusing by the array of reference standards used to quantify β-hCG. As shown by Fossum and colleagues, the appearance of these structures can be correlated with β-human chorionic gonadotropin (β-hCG) levels (Table 2). 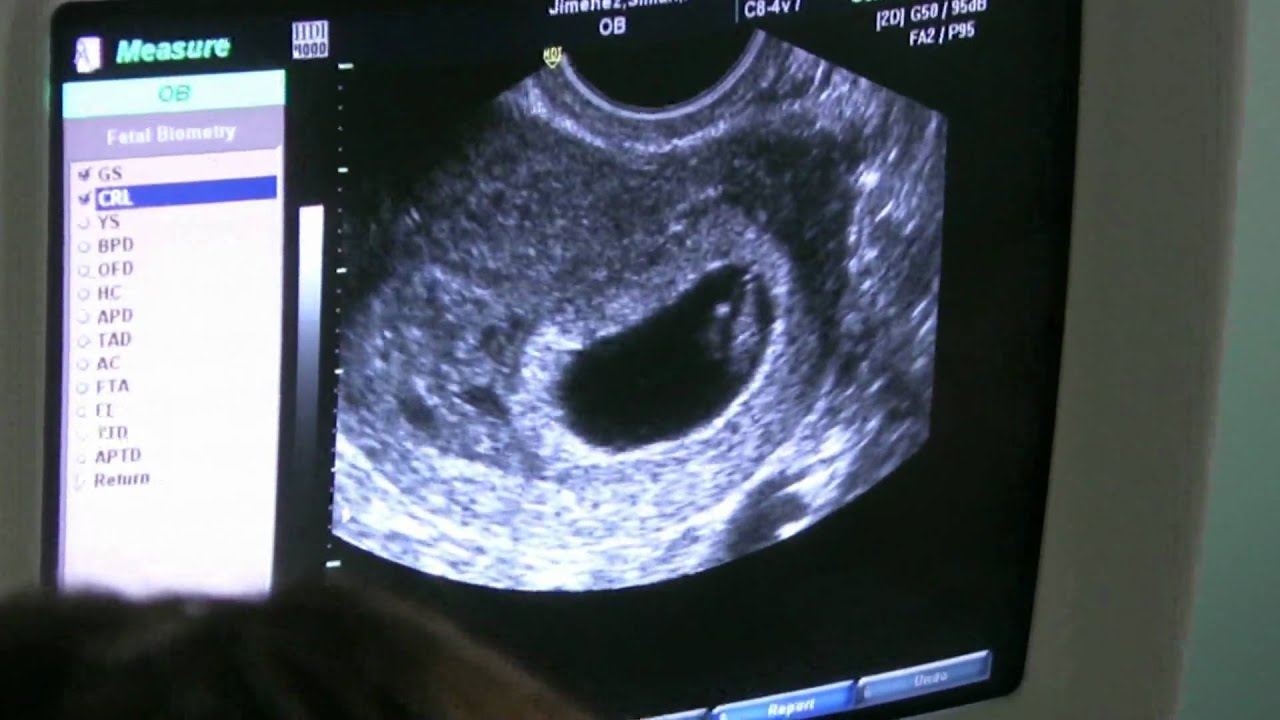
A fetal pole with heart tones is typically seen by the completion of 7 menstrual weeks (Fig 1D). A yolk sac is usually seen by 6 menstrual weeks, or by the time the mean diameter of the sac has reached 10 mm (Fig 1B and Fig 1C). 1 With a transvaginal probe, a 2- to 3-mm gestational sac can usually be seen by 5 weeks from the last menstrual period (Fig 1A). Warren and associates described the orderly appearance of gestational sac, yolk sac, and embryo with heartbeat at a given number of days from the onset of the last menstrual period (Table 1). 
Alternatively for international readers, the website,, of The International Society of Ultrasound in Obstetrics and Gynecology should be searched for similar guidelines. For United States readers, the website,, of the American Institute of Ultrasound in Medicine will be helpful for guidelines. This includes, but is not limited to, power settings, basic orientation, and proper cleaning of ultrasound probes between uses. The role of the early anatomic survey, when free DNA screening for chromosomal anomalies is being utilized, remains to be determined.Īny health-care provider performing diagnostic ultrasound must understand the physics of diagnostic ultrasound and have thorough, supervised training. The disadvantages are cost, decreased sensitivity for major anomalies compared to the 20 week exam, and marked increase in training requirements for providers. Similarly the standard of care for performing routine ultrasound at 12–14 weeks' gestation from the LMP varies from country to country. Early identification of C-section scar pregnancy.Early diagnosis of major trisomies as part of nuchal screening.Early diagnosis of certain severe and lethal anomalies.The potential benefits of a subsequent ultrasound examination at 12–14 weeks from the LMP include: The disadvantages of performing this examination routinely are related to cost, errors in diagnosing ectopic pregnancies that in fact are intrauterine, increased training requirements for providers, and potential biologic hazards to the fetus that are presently unknown. The standard of care for performing routine ultrasound examination at 6–7 weeks varies from country to country. Early identification of multiple gestation and correct determination of chorionicity.Identification of missed abortion, ectopic pregnancy, and C-section scar pregnancies.Correct dating of gestational age since 10–15% of women will have inaccurate assignment of gestational age of more than 1 week based on menstrual history.The benefits of routine transvaginal ultrasound at 6–7 weeks from the LMP include: Failure to understand the limitations of diagnostic ultrasound or inadequate training of physicians in this technique can result in grave complications for the patient and liability for health-care providers. In fact, certification of residency programs in many countries requires documentation of adequate exposure to and training in the evaluation of first-trimester ultrasound. Today's obstetrician gynecologist is required to interpret and in many cases perform ultrasound scans in the first trimester.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
